Orthopaedic guidelines generally recommend same-day clinical assessment when certain features are present following a lower leg injury. The information below is intended to help you understand what to discuss with a medical professional — not to replace that assessment. If you are in significant pain or unable to weight-bear, please attend an emergency department.
What Does a Ruptured Achilles Tendon Feel Like?
In the medical literature, patients who have sustained a complete Achilles tendon rupture commonly describe the moment of injury as a sudden, forceful sensation at the back of the lower leg — frequently likened to being struck from behind. An audible pop or crack is reported in a significant proportion of cases.
Ruptures most frequently occur during explosive movements such as sprinting, jumping, or sudden changes of direction — but clinical literature also documents ruptures occurring during more everyday activities including stepping off a kerb or descending stairs. Achilles rupture is not exclusively a sporting injury.
"I genuinely thought someone had hit me from behind. I turned around and nobody was there."
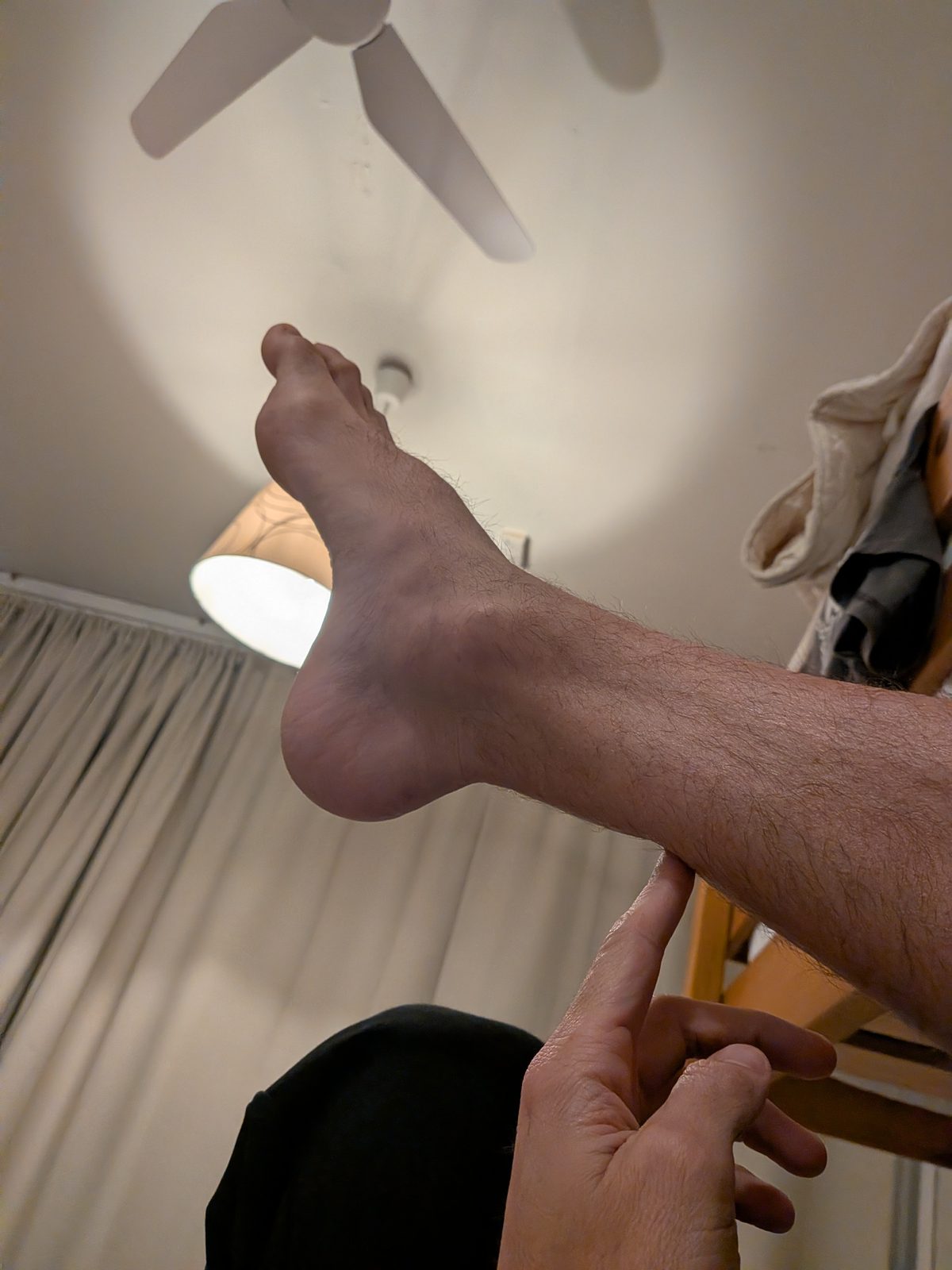
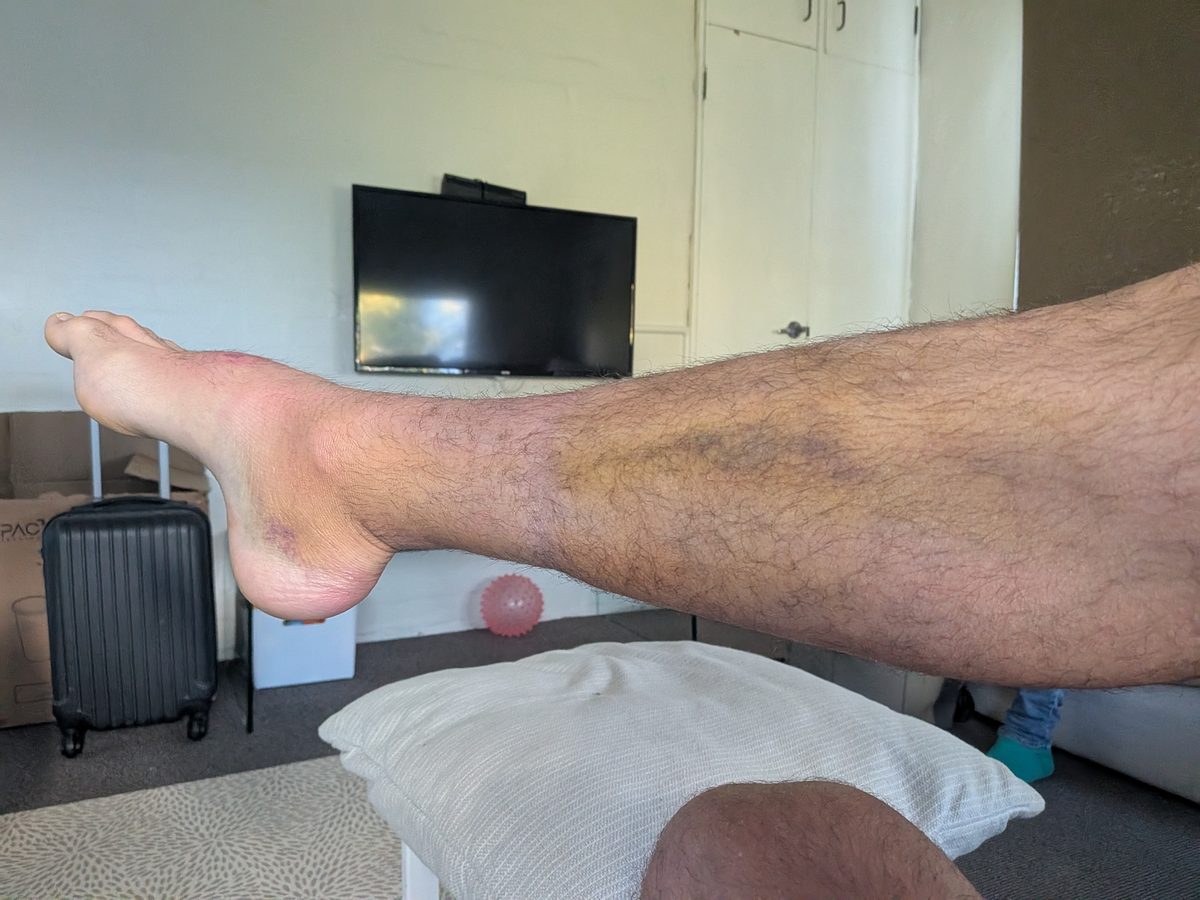
One aspect that frequently surprises people — and that clinicians routinely highlight — is that many individuals with a complete rupture find they can still walk to some degree. Other muscles of the lower leg can partially compensate for the lost tendon function in the short term. The ability to walk does not rule out a complete rupture and should not be used as a basis for deciding whether to seek medical attention.
What Are the Symptoms of an Achilles Tendon Rupture?
The following signs and symptoms are commonly described in clinical literature on Achilles tendon rupture. Their presence or absence in any individual case cannot confirm or exclude a diagnosis — that requires clinical assessment. This information is provided to help readers communicate their symptoms more clearly when they consult a healthcare professional.
An audible or felt crack at the moment of injury is reported in approximately 70% of complete ruptures in the literature. Clinicians note that its absence does not exclude a rupture.
Clinicians commonly assess whether a patient can rise onto tiptoe on the affected side. In complete ruptures, this is typically not possible. Partial ruptures may retain some tiptoe function.
A visible or palpable depression in the tendon approximately 2–6cm above the heel is a commonly reported finding. Significant swelling in the hours following injury may obscure this gap.
The ability to point the foot downward (plantarflexion) is significantly weakened or absent following a complete rupture. The degree of pain is variable and is not a reliable indicator of severity.
Localised swelling above the heel typically develops following a rupture. Bruising may track toward the foot over 24–48 hours. Neither is present in all cases immediately after injury.
As noted in clinical guidelines, many people with a complete Achilles rupture can still walk with a limp. Retained walking ability is not a reliable indicator that a rupture has not occurred.
Clinical literature consistently notes that pain severity following Achilles rupture does not correspond to injury severity. A complete rupture may produce less acute pain than a partial tear, because tension in the tendon is released at the moment of rupture. Pain level alone should not be used to decide whether to seek medical care.
How Is the Thompson Test Performed — and What Does It Show?
The Thompson test (also referred to as the Simmonds-Thompson test) is a bedside clinical assessment used by healthcare professionals to evaluate Achilles tendon integrity. It is one of the primary tools clinicians use in initial assessment of a suspected rupture. Understanding how it works may help readers ask informed questions at a medical appointment.
The test is performed by a clinician. A self-assessment result should not be used as the basis for any treatment decision.
The patient lies face down (prone) on an examination table, with both feet hanging unsupported off the edge. This position removes active muscle compensation from the assessment.
The clinician firmly compresses the calf muscle — the muscular bulk of the lower leg, not the tendon itself. A firm compression is required for a reliable result.
The clinician observes whether the foot moves in response to the compression. The presence or absence of foot movement informs the assessment of tendon continuity.
The foot plantarflexes (moves downward) when the calf is compressed, indicating an intact mechanical connection. This suggests no complete rupture — though partial tears or other injury are not excluded.
The foot does not move, or moves minimally, when the calf is compressed. Clinicians interpret this as indicating disruption of tendon continuity. A positive result is considered a significant clinical finding warranting urgent further assessment.
Peer-reviewed literature reports sensitivity of approximately 96% and specificity of approximately 93% for the Thompson test in diagnosing complete Achilles rupture (Maffulli, 1998). Clinicians generally regard it as reliable for initial triage. Imaging is typically required before any treatment decision is finalised. A negative Thompson test does not exclude partial tears.
What Conditions Can Be Mistaken for an Achilles Rupture?
Several conditions can present with symptoms that overlap with Achilles tendon rupture. Differentiation requires clinical assessment and in many cases imaging. The table below is general background information to help readers understand what a clinician may be considering — it is not a diagnostic tool.
| Condition | Common presentation | Thompson test | Clinical urgency |
|---|---|---|---|
Complete Achilles Rupture |
Sudden pop, acute weakness, palpable gap, unable to tiptoe | Typically positive | Emergency — same-day assessment generally recommended |
Partial Achilles Tear |
Acute pain and swelling, weakness with retained function. Often no pop. | Typically negative | Urgent — assessment within 24–48 hours generally recommended |
Achilles Tendinopathy |
Gradual onset, morning stiffness, pain with loading — no acute injury event | Negative | GP appointment generally appropriate |
Plantaris Muscle Rupture |
Sudden medial calf pain, function typically preserved | Negative | GP or sports medicine assessment |
High-Grade Ankle Sprain |
Lateral ankle pain and swelling, typically inversion mechanism | Negative | Emergency or urgent care assessment |
Calcaneal (Heel) Fracture |
Impact or fall mechanism, diffuse heel pain, difficulty weight-bearing | Negative | Emergency — imaging required |
How Do You Know If You Have a Partial Achilles Tear Instead of a Full Rupture?
Partial Achilles tendon tears are generally more difficult to diagnose than complete ruptures, as the classic presentation is typically absent. Some plantarflexion is preserved and pain is variable. Partial tears are sometimes initially assessed as severe tendinopathy.
Clinical literature notes that when significant localised tenderness, swelling, or weakness is present following an acute injury event — even without an audible pop — imaging is generally recommended to exclude a partial rupture. An unidentified partial tear subjected to ongoing load may progress to a complete rupture.
What Signs Suggest a Partial Achilles Tear Rather Than a Complete Rupture?
- Acute onset during an activity, without an audible pop
- Localised tenderness over the tendon approximately 2–6cm above the heel
- Weakness in plantarflexion that does not represent a complete loss of function
- Swelling localised to the tendon rather than the ankle joint
- Pain that is more pronounced when descending stairs or on decline surfaces
Should I Go to Emergency If I Think I've Ruptured My Achilles?
Orthopaedic guidelines and clinical literature consistently recommend prompt assessment — generally on the same day — when certain features are present following a lower leg injury. The following list reflects what major clinical guidelines describe as indicators for urgent emergency department attendance. This is not a personal recommendation from this website — it is a summary of what published clinical guidelines advise.
- An audible or felt pop at the back of the ankle or lower leg at the time of injury
- Inability to rise onto tiptoe on the affected side
- A visible or palpable gap or depression above the heel
- Absence of foot movement when the calf is compressed (positive Thompson test result)
- Sudden significant weakness in the lower leg following an explosive or unexpected movement
Orthopaedic literature generally notes that when surgical repair is being considered, outcomes are more favourable when assessment and intervention occur early — commonly cited as within 72 hours of injury. After this period, tendon retraction and tissue changes may increase surgical complexity. This is a matter for a surgeon to assess and discuss with you. The information is provided here so readers understand why published guidelines recommend prompt clinical review.
Why Timing Matters for Treatment Options
An Achilles tendon rupture is a time-sensitive injury — not in the sense of a surgical emergency requiring immediate theatre, but in the sense that the biological window for optimal non-surgical management is narrow, and delays affect both surgical and conservative treatment pathways.
What happens in the first days after rupture
In the hours immediately after an Achilles tendon rupture, a haematoma — a clot of blood — forms at the rupture site. This clot acts as a temporary scaffold, holding the torn tendon ends in relatively close proximity. It also contains growth factors that initiate the early healing cascade. The inflammatory phase of tendon healing begins within the first 24–48 hours.
Over the following days, progressive oedema (swelling) develops in and around the tendon sheath. As swelling increases, the space between the tendon ends widens. The haematoma begins to organise into fibrous tissue. The tendon ends, which were initially relatively approximated, begin to retract as the swelling separates them.
This progression is the biological basis for the clinical convention that earlier assessment leads to better non-surgical outcomes — the earlier the foot is placed in plantarflexion to approximate the tendon ends, the closer together those ends are when they are held in position.
What "acute" versus "delayed" presentation means clinically
Published orthopaedic literature uses specific terminology to describe presentation timing after Achilles rupture. Understanding these definitions helps you interpret clinical guidance:
- Acute presentation: Generally defined as assessment and treatment within 2 weeks of injury. Both surgical and conservative management can be performed with good outcomes in this window, though earlier is better for conservative management specifically.
- Sub-acute presentation: 2–4 weeks after injury. Conservative management becomes more challenging as the tendon ends have retracted further. Surgical repair remains technically feasible but more complex due to tissue changes.
- Delayed or neglected presentation: Beyond 4–6 weeks. The tendon ends have typically retracted significantly and fibrous tissue has filled the gap. Surgical management at this stage may require tendon lengthening procedures or tendon grafting rather than primary repair — substantially more complex operations with longer recovery timelines.
Why people miss the early assessment window
Delayed presentation after Achilles rupture is more common than clinicians would prefer — and the reasons are well-documented. The most common is misdiagnosis: approximately 20–25% of Achilles ruptures are initially missed, most commonly because the person can still walk and weight-bear on the injured leg. The ability to walk does not exclude a complete Achilles tendon rupture — the plantaris and toe flexors provide enough residual function for limited weight-bearing even with a complete Achilles rupture.
Other common reasons for delayed presentation include attributing the injury to a sprain or "popped calf," waiting for a GP appointment rather than attending emergency assessment, or walking it off and hoping it would resolve. If you are reading this page and recognise these scenarios in your own recent injury, the practical advice is the same regardless of how much time has passed: seek orthopaedic assessment as soon as possible. Earlier is better — but there is no time at which assessment becomes pointless.
This is the most important point for understanding why Achilles ruptures are so commonly missed. The calf-Achilles complex is not the only structure capable of plantarflexion — the toe flexors and plantaris contribute enough residual function to allow limited walking even with a complete Achilles tear. A person who limps into an emergency department under their own power may have a complete rupture. The Thompson test and imaging, not the ability to walk, are the appropriate diagnostic tools.
What Imaging Is Used to Diagnose an Achilles Tendon Rupture?
Clinical assessment — including the Thompson test — is typically sufficient to inform an initial triage decision. Medical guidelines generally require imaging before a definitive treatment pathway is determined. The following describes how each modality is typically used, based on published clinical practice guidelines.
Ultrasound
Ultrasound is described in most Australian and international clinical guidelines as the preferred first-line imaging investigation for suspected Achilles tendon rupture. It is real-time, widely available, and — in experienced hands — highly accurate. Clinicians use it to confirm rupture, assess gap size, and determine whether tendon ends approximate in plantarflexion, which informs the treatment pathway discussion.
MRI
MRI provides the most detailed assessment of soft tissue integrity. It is typically used when ultrasound findings are inconclusive, when a partial tear is suspected, or when the clinical picture is unclear. It is generally not required for straightforward complete ruptures where ultrasound is diagnostic.
X-ray
Plain radiography cannot visualise soft tissue structures and cannot diagnose an Achilles tendon rupture. Clinicians may use X-ray to exclude associated bony injuries — such as calcaneal avulsion fractures — which can occasionally occur with a similar mechanism.
What Should I Do Next After a Suspected Achilles Rupture?
If you have read this page and are concerned you may have sustained an Achilles tendon injury, the most important step is to seek professional clinical assessment. The following reflects what orthopaedic and emergency medicine guidelines generally describe — it is not personal medical advice from this website.

- Most guidelines recommend avoiding weight-bearing on the injured leg until it has been assessed by a clinician
- First aid guidelines generally suggest applying ice wrapped in cloth to reduce swelling — typically 20 minutes on, 20 minutes off
- Elevating the leg where possible is commonly recommended to help manage swelling
- If the symptoms described in clinical guidelines are present, attending an emergency department or contacting an orthopaedic surgeon is generally recommended — same-day assessment is typically advised
- When seen by a clinician, it may be useful to ask whether a Thompson test will be performed if it has not been mentioned
- Asking your treating clinician about the role of imaging in confirming the diagnosis is reasonable
- Asking your treating clinician to explain both surgical and non-surgical treatment options will help you make an informed decision about your care
This page provides general health information only. It is compiled from peer-reviewed medical literature and published clinical guidelines and is intended to help readers understand common clinical presentations, terminology, and treatment pathways.
The content on this page does not constitute medical advice and does not create a clinical or professional relationship between the reader and this website or its authors. It cannot and should not be used to self-diagnose, self-treat, or make treatment decisions without consulting a qualified healthcare professional.
Every individual's injury, health history, and circumstances are different. Only a qualified clinician — such as an orthopaedic surgeon, sports medicine physician, or physiotherapist — can assess your specific situation and provide appropriate medical advice.
If you believe you may have sustained an Achilles tendon rupture or any other serious injury, please seek professional medical assessment promptly. If you are in doubt, attend an emergency department.
Some links on this site are affiliate links. If you purchase a product through these links, this site may earn a small commission at no additional cost to you. Affiliate relationships do not influence the health information provided on this or any other page.